Welcome to Nevada Vein & Vascular
Providing A Broad Range Of Vascular Surgery & Vein Management Services
Welcome to Nevada Vein & Vascular
Providing A Broad Range Of Vascular Surgery & Vein Management Services
We are devoted to providing quality patient care on all levels.
At our practice in Reno, Nevada, we want you to be educated about your vascular problems and work with you in making decisions about your care. Our board-certified surgeon, Dr. Janet Albright has many years of experience and prides herself on patient-centered care.
Diseases We Treat
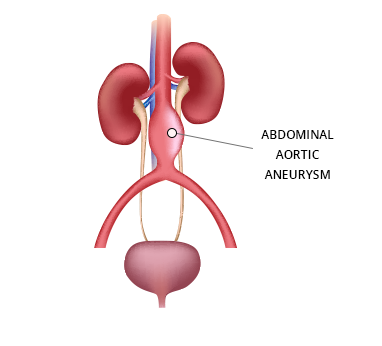
What is an Aneurysm?
An aneurysm occurs when part of an artery wall weakens, allowing it to balloon out or widen abnormally.
Types of Aneurysm
Aortic Occlusive Disease
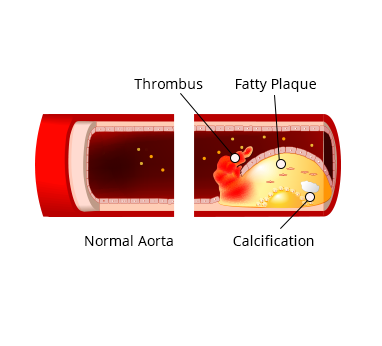
Aortic Occlusive Disease occurs when blood flow in the aorta is blocked. There are many different health conditions that can cause blockages in the aorta.
Aortic Occlusive Disease can slow or block blood flow to the body’s major organs and cause a number of serious health issues.
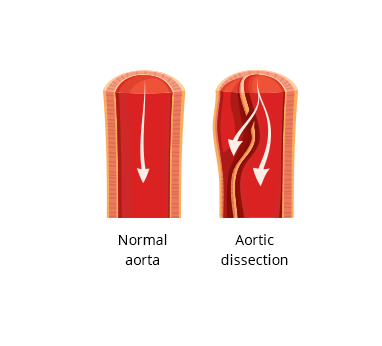
Aortic Dissection (AD)
Aortic dissection (AD) occurs when an injury to the innermost layer of the aorta allows blood to flow between the layers of the aortic wall, forcing the layers apart.
In most cases, this is associated with a sudden onset of severe chest or back pain, often described as “tearing” in character.
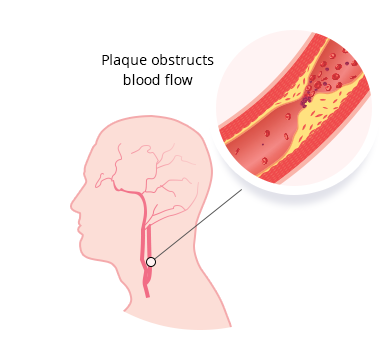
What is Carotid Artery Disease?
Carotid artery disease is a disease in which a waxy substance called plaque builds up inside the carotid arteries.
What causes Carotid Artery Disease?
Carotid artery disease is caused by a buildup of plaque in arteries that deliver blood to your brain. Plaques are clumps of cholesterol, calcium, fibrous tissue.
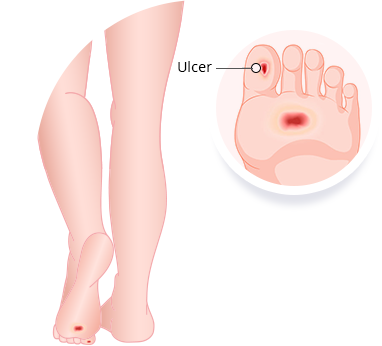
What is a Diabetic Foot Wound and Limb Salvage?
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes and is commonly located on the bottom of the foot.
Foot ulceration precedes 85 percent of diabetes-related amputations. Research has shown, however, that development of a foot ulcer is preventable.
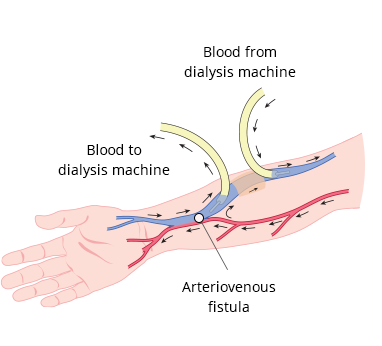
What is Dialysis Access?
A hemodialysis access, or vascular access, is a way to reach the blood for hemodialysis.
The access allows blood to travel through soft tubes to the dialysis machine where it is cleaned as it passes through a special filter, called a dialyzer.
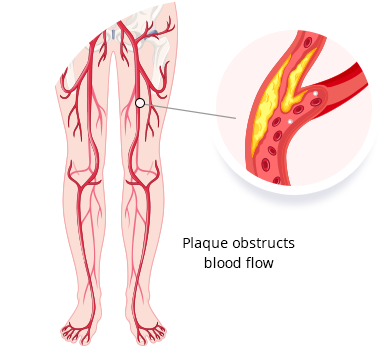
What is Peripheral Arterial Disease?
Peripheral Arterial Disease is a common circulatory problem in which narrowed arteries reduce blood flow to your limbs.
Types of Peripheral Arterial Disease
- Lower Extremity
- Upper Extremity
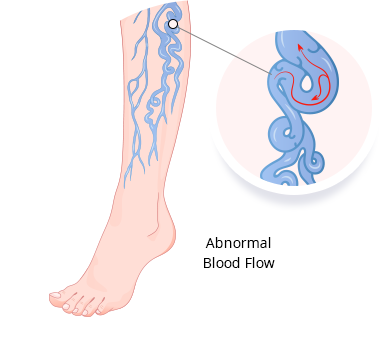
What is Venous Disease?
The most common causes of venous disease are previous cases of blood clots and varicose veins.
Types of Venous Disease
Diseases We Treat
What is an Aneurysm?
An aneurysm occurs when part of an artery wall weakens, allowing it to balloon out or widen abnormally.
Types of Aneurysm

Aortic Occlusive Disease
Aortic Occlusive Disease occurs when blood flow in the aorta is blocked. There are many different health conditions that can cause blockages in the aorta.
Aortic Occlusive Disease can slow or block blood flow to the body’s major organs and cause a number of serious health issues.

Aortic Dissection (AD)
Aortic dissection (AD) occurs when an injury to the innermost layer of the aorta allows blood to flow between the layers of the aortic wall, forcing the layers apart.
In most cases, this is associated with a sudden onset of severe chest or back pain, often described as “tearing” in character.

What is Carotid Artery Disease?
Carotid artery disease is a disease in which a waxy substance called plaque builds up inside the carotid arteries.
What causes Carotid Artery Disease?
Carotid artery disease is caused by a buildup of plaque in arteries that deliver blood to your brain. Plaques are clumps of cholesterol, calcium, fibrous tissue.

What is a Diabetic Foot Wound and Limb Salvage?
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes and is commonly located on the bottom of the foot.
Foot ulceration precedes 85 percent of diabetes-related amputations. Research has shown, however, that development of a foot ulcer is preventable.

What is Dialysis Access?
A hemodialysis access, or vascular access, is a way to reach the blood for hemodialysis.
The access allows blood to travel through soft tubes to the dialysis machine where it is cleaned as it passes through a special filter, called a dialyzer.

What is Peripheral Arterial Disease?
Peripheral Arterial Disease is a common circulatory problem in which narrowed arteries reduce blood flow to your limbs.
Types of Peripheral Arterial Disease
- Lower Extremity
- Upper Extremity

What is Venous Disease?
The most common causes of venous disease are previous cases of blood clots and varicose veins.
Types of Venous Disease

Candice WDr. Albright and her staff are extremely caring professionals. When worry took over, Dr. Albright did not hesitate to call me in the evening to ease my mind. She and Melissa go out of their way to make their patients feel safe and well-cared for during the entire process. They understand the stress and worry for patients and do not hesitate to respond very quickly if an issue or question arises. The surgery was successful, and above everything, Dr. Albright is the type of doctor everyone would love to have – she’s a normal, caring person. No ego involved! Just a great smile and caring manner!
Our Providers
Every patient is unique and treated as such. The vascular system is intriguing – making the best of your arteries and veins is what makes our practice happen. We offer a variety of vascular services including treatment for Abdominal Aortic Aneurysm, Lower Extremity Arterial Disease, and Peripheral Arterial Disease (PAD). We also offer vein treatment options for Vein Disease including Sclerotherapy and Laser Ablation.
Our doctors as well as our Physician Assistant, Terri Elliot are excited to provide help wherever needed. Individualized treatment for every patient is our goal at Nevada Vein and Vascular.
