The carotid arteries are a pair of blood vessels, one on each side of the neck, within the soft tissues. These arteries begin in the chest as a single common carotid artery and then branch in the neck into internal and external carotid arteries. The external carotids supply muscles in the neck, face, and scalp but the internal carotid continues without any branches into the brain. When we talk about carotid artery disease, it is always in reference to the internal carotid artery because all symptoms and treatments are focused on this vessel.
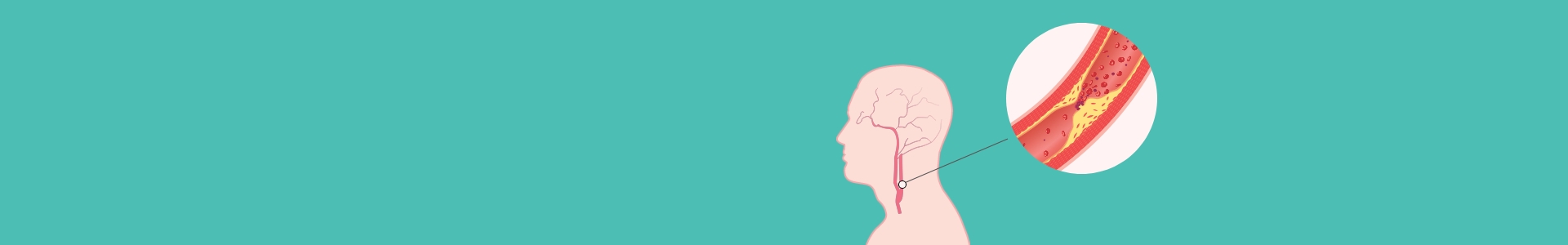
Carotid Artery Disease
Carotid Artery Disease
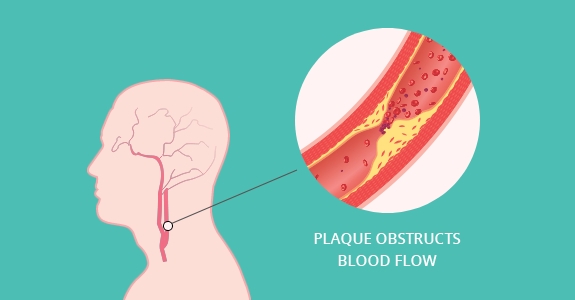
Carotid Stenosis
Carotid artery disease is also called carotid artery stenosis. Stenosis is the medical term for narrowing, or blockage and it can be used to refer to a blockage in any blood vessel. As in any blood vessel, the narrowing is caused by atherosclerosis, or build-up of plaque and hardening of the arteries. Atherosclerotic plaque is an accumulation of cholesterol within the wall of the artery. As the plaque builds up, the narrowing becomes more severe and the plaque is more likely to fracture, break off, and travel through the internal carotid artery to brain. This results in a stroke.
What Are Symptoms Of Carotid Artery Disease?
Vascular disease in other parts of the body is likely to cause symptoms as a blockage becomes more severe. In the legs, patients often notice progressive pain with walking. In the kidneys, arterial blockage may lead to high blood pressure or declining kidney function. In the intestines, one may develop abdominal pain after eating. The carotid artery is different in that the first indication of a problem may be a mini-stroke, or TIA (transient ischemic attack), or a major disabling stroke with permanent deficits.
Transient Ischemic Attack (TIA)
By definition, symptoms of a TIA resolve completely within 24 hours of onset. In reality, most TIA symptoms resolve within a few minutes. If symptoms do not resolve within a day, a person is considered to have had a stroke. Symptoms depend on which part of the brain is affected, but when attributed to the carotid artery, they most commonly include one or more of the following:
- Temporary loss of vision
- Slurred speech
- Inability to speak or form words
- Numbness or tingling in an arm or leg
- Paralysis of an arm or leg
Many patients describe a “gray shade” coming down over the eye which resolves in a few minutes.
Stroke symptoms are identical, but may be more severe and do not resolve.
If any of these symptoms develop, you should call 911 immediately as it is not possible to predict whether a TIA will evolve into a major stroke and there are interventions which can be done if you reach the hospital in time.
How Is Carotid Artery Disease Diagnosed?
Carotid disease is usually diagnosed with a non-invasive ultrasound test called a carotid duplex exam (link to NIV section). Ideally, carotid disease is identified before a patient has a TIA or stroke. Certain risk factors predispose to the development of carotid stenosis and in patients with risk factors, physicians may order a screening exam.
Risk factors include:
- Smoking
- Hypertension (high blood pressure)
- High cholesterol
- Coronary artery disease
- Smoking
- Family history of stroke
- History of head/neck radiation
Once diagnosed, carotid artery disease is classified as mild, moderate, and severe depending on the percent stenosis. Mild is 1-49%, moderate is 50-69%, and severe is generally considered any blockage over 70%.
At Nevada Vein and Vascular, we perform carotid screening ultrasounds and offer all of our patients surveillance imaging in accordance with Society of Vascular Surgery guidelines.
If you or a family member have risk factors for carotid disease or have a history of TIA/stroke, please call us at (775) 323-3000 to schedule an appointment.
How is Carotid Disease Managed or Treated?
Patients with carotid disease should be evaluated by a vascular surgeon because surveillance is important. If a patient is found to have mild or moderate disease, surveillance ultrasounds should be performed every 6 months to one year. It is also important to start the proper medication regimen to decrease the chance of having a stroke and slow the progression of the disease. In some cases, it may be possible to avoid surgery completely.
Patients with high-grade or severe disease, or those who have had a TIA or stroke are generally considered for surgery. Please click below to learn about treatment options for carotid disease.
Carotid Endarterectomy (CEA)
Carotid Artery Stenting
Carotid Endarterectomy (CEA)
Carotid endarterectomy, or CEA, is the standard treatment for high-grade carotid stenosis. Performed through an incision on the neck, the carotid artery is opened and the plaque is extracted. The artery is then patched to ensure it remains wide open. Patients are admitted to the hospital, but most are able to go home the following day.
Carotid Artery Stenting
Carotid artery stenting, or CAS, is a minimally invasive option in which a stent is inserted from the femoral artery in the groin into the carotid artery. Prior to stent placement, a separate device called a filter, is temporarily inserted to decrease the risk of stroke. Once the stent is placed, the filter is removed. The procedure is performed without general anesthesia and usually requires one night in the hospital.
