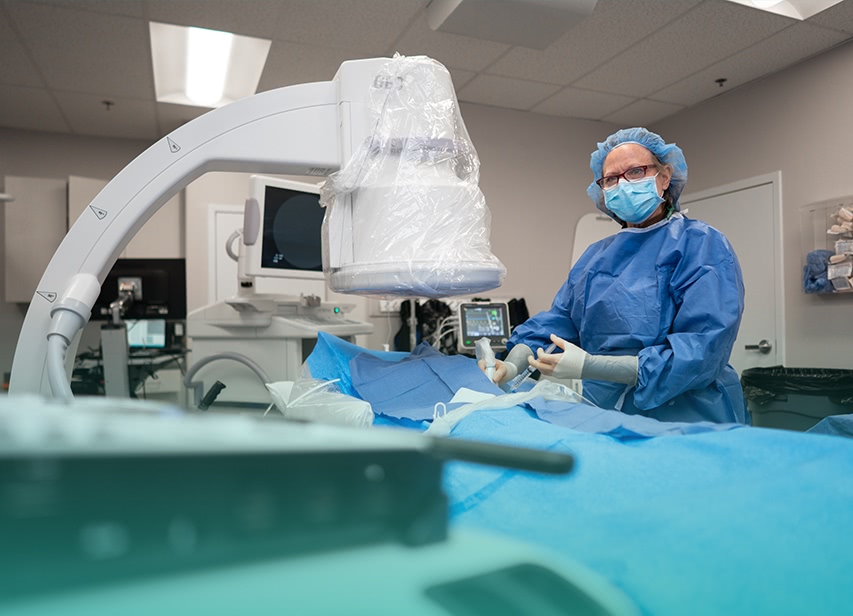
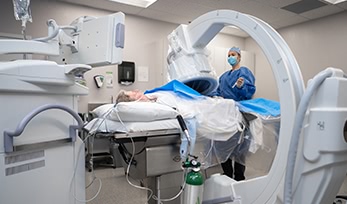
In early 2019, Nevada Vein and Vascular completed the build-out of Reno’s first Office-based Interventional Suite, or OIS. An OIS is a specialized room where minimally-invasive endovascular procedures are performed. Our state-of-the-art facility incorporates the latest in imaging technology and is fully-stocked with a large variety of tools which allow us to perform both simple and complex peripheral vascular interventions that would otherwise need to be done in the hospital.
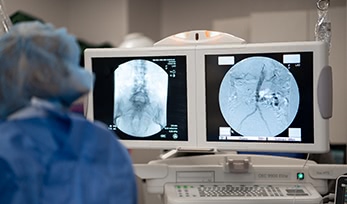
We perform a wide variety of diagnostic and therapeutic interventions in the OIS including diagnostic angiography, abdominal and lower extremity endovascular revascularizations including complex limb salvage procedures, iliac stenting, upper extremity angiography, and fistulograms with interventions for dialysis patients.
These same day procedures are completed under minimal to moderate conscious sedation. Our trained staff and physicians continuously monitor patients during the procedure and throughout their recovery to provide a safe experience and allow a quick recovery and return home with minimal to no side effects.

 We offer the best outpatient experience possible by providing timely access to the care you need, tailored to your specific condition. Our knowledgeable staff is dedicated to our patients and every procedure is performed with meticulous attention to detail.
We offer the best outpatient experience possible by providing timely access to the care you need, tailored to your specific condition. Our knowledgeable staff is dedicated to our patients and every procedure is performed with meticulous attention to detail. In medical jargon, endo simply means “inside” and “vascular” implies arteries or veins. An endovascular procedure is one which is performed within the blood vessel itself.
In medical jargon, endo simply means “inside” and “vascular” implies arteries or veins. An endovascular procedure is one which is performed within the blood vessel itself.