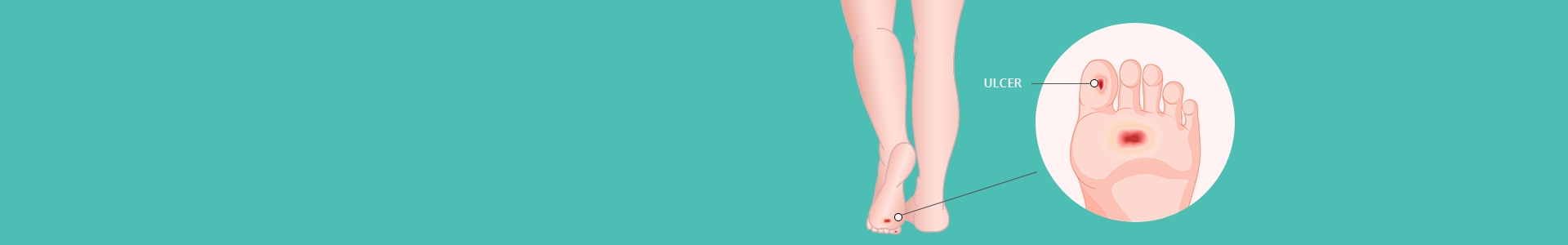
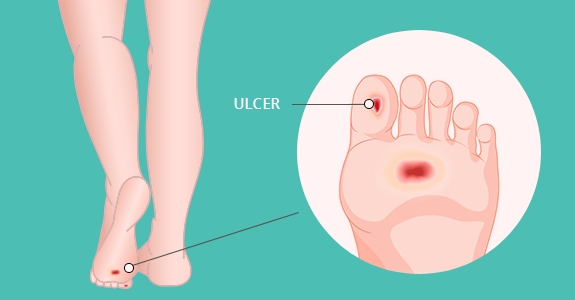
Long-standing diabetes takes a toll on the entire cardiovascular system. In the legs, chronically-elevated blood sugar particularly affects the nervous system, leading to peripheral neuropathy, the small arteries below the knee, and micro-circulation in the foot.
Over time, neuropathy leads to joint deformities in the toes and, “neuropathic ulcers” on the plantar surface (the bottom of the foot). Diabetes also contributes to PAD, and when combined with peripheral neuropathy, the two conditions can lead to diabetic foot wounds, infection, gangrene, and ultimately, amputation.
Once a foot wound develops in a patient with diabetes, the risk of limb-loss escalates. Without aggressive, and sometimes urgent treatment, gangrene may set in. Treatment of diabetic foot wounds and vascular disease requires specific expertise, so much so that the field of “limb salvage” was developed because the rates of amputation are unacceptably high.
Dr. Albright has a specific interest and expertise in diabetic limb salvage. Dr. Albright takes a proactive approach in the diagnosis, management, and follow-up of this condition. Dr. Albright is the director of the wound clinic at Renown. She evaluates and treats hundreds of diabetic foot wounds each year.
At NVV, we believe amputation is a last resort. Because of our philosophy and proactive approach, we are frequently asked to provide second opinions regarding options for limb salvage.
If you or a family member has diabetes, please give us a call to set up a consultation. Diabetic patients should be screened for vascular disease, and in most cases, insurance will cover the examination. We firmly believe the best way to treat a diabetic foot wound is to prevent it from occurring in the first place.